Re L and M (Children) [2013] EWHC 1569 (Fam)
http://www.bailii.org/ew/cases/EWHC/Fam/2013/1569.html
This case, in which I represent the father, was the retrial of a finding of fact hearing (following a successful appeal). Additional medical expert evidence assisted in concluding there were fewer fractures to the child’s skull than originally thought.
In relation to the instruction of medical experts, Baker J was clear that:
“[i]n difficult cases of non-accidental injury, it will continue to be the case that expert evidence from a variety of disciplines will be necessary to assist the court to resolve the proceedings.”
The medical evidence given in this case (written and oral) points to a continually evolving picture and serves as a reminder that “…that today’s medical certainty may be discarded by the next generation of experts or that scientific research would throw a light into corners that are at present dark” (Dame Butler-Sloss).
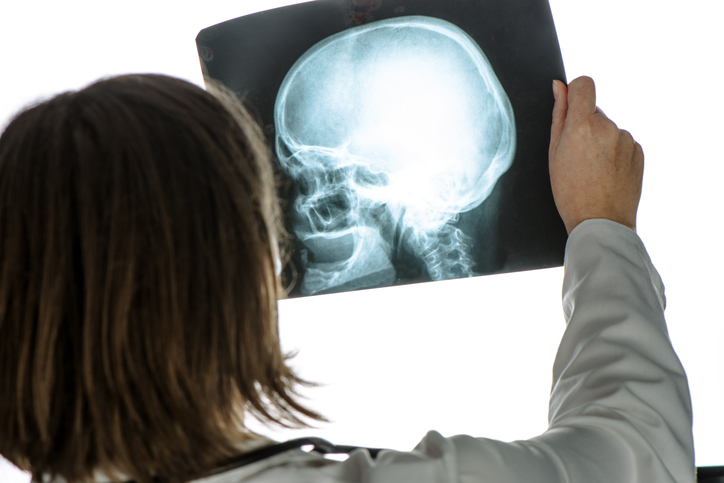
Due to the nature of the skull fracturing, considerable time was spent considering which lucencies (lines on the x-ray) were fractures and which were fissures or accessory sutures. Some key areas which were dealt with are briefly detailed below:
Fissures
- What is a fissure? The skull consists of a number of plate like bones which are joined together by fibrous areas which allow a little bit if movement, these are called sutures. Sometimes there are other areas where the bone is not so hard or not joined well and we call these fissures (incomplete ossification). These are seen commonly next to the sagittal suture. As a child gets older, they will gradually disappear.
- It is thought that fissures are not uncommon but the reality is (as accepted by many experts) that we simply don’t know the true number of skull fracture or of fissures (as many children are not x-rayed).
- It is accepted that many fissures have probably been diagnosed as fractures in the past. This is of course concerning when you consider the consequences of such. As one expert put it: “A worry in my mind – how often are we overcalling fractures?”
- A fissure is usually short, linear, not angulated or branching, perpendicular to the adjacent suture and has no evidence of swelling.
- There is no specific association between a fissure and a fracture but a fissure may mean lesser force is required to fracture than if there was no fissure. There is no literature or research to back this up but as fissures contain under-developed fibrous tissue their very presence presumably means that the area in which the fissure is located is weaker than if it was a normal, complete plate of bone (fully ossified).
- The possibility that a fracture arose from a fissure (i.e. Started as a fissure and after force is applied (probably less force) it became a fracture) cannot be excluded.
- That would mean the presence of fissures could lead to fractures extending from them with a lesser degree of force.
- If that is the case then widening of a pre-existing fissure could look just the same as a primary fracture.
- Usually we only see one or two fissures on a skull; more would be unusual but again the true number is unknown as they are not looked for.
- A traumatised fissure describes a fissure that has experienced some kind of injury/force that then looks like a fracture on a scan.
Fractures
- In terms of degree of force, we do not know what is required. Not all infants who have trauma are sent for scans so we don’t even know the true number of fractures. Everyday clinical experience leads us to believe force won’t be trivial and is probably significant force.
- The commonest fracture in accidental and NAI is a simple linear fracture. More complex fractures are more commonly seen in context of NAI but it is the case that the appearance of a fracture is likely to relate to the degree of force rather than allowing us to make a distinction between accidental and NAI.
- A complex fracture can include: separation of fracture margins, a branching fracture, an occipital bone fracture or bilateral fractures.
- Similarly, for the same reasons as described above, a skull will be more vulnerable to further fracture where it already has a fracture. It is a biologically plausible mechanism where if a fracture is present and further force is applied, the fracture may extend. It would not, however, be likely to cause a general vulnerability across whole skull.
- The cause of scalp swelling isn’t fully understood due to a lack of research but is thought to be two-fold: the trauma itself having damaged the soft tissues but also when the bone breaks some blood and fluid will escape from ends of bone.
